How safe is the Pfizer vaccine and how was it done so quickly?
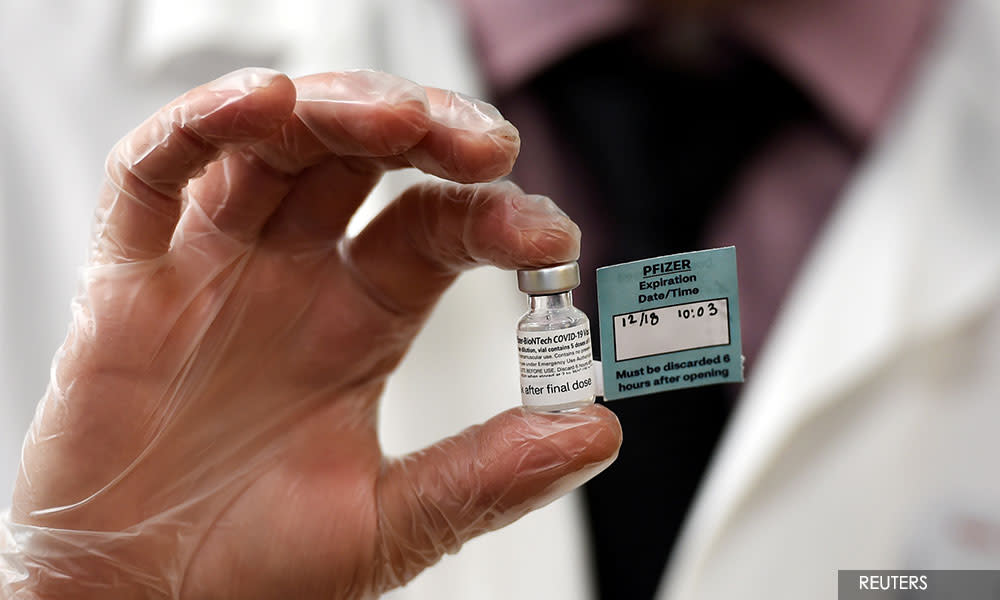
KINIGUIDE | In the year-long battle against Covid-19, researchers have worked hard to create a vaccine against the coronavirus which has killed nearly two million people across the globe.
The pharmaceutical companies have accelerated the vaccine development process and succeeded in coming up with several promising vaccines within months instead of years.
This extraordinary feat, however, sparked questions among sceptics on the safety and efficacy of the vaccines.
Many of these sceptics include Malaysians themselves. Debate on social media has intensified regarding the safety of Covid-19 vaccines with many expressing concern that the vaccine development process has been rushed.
WATCH: Can I trust the vaccine? An expert's view on the matter
The first batch of Covid-19 vaccines is expected to arrive in late February – part of an order for 12.8 million doses of a vaccine co-developed by Pfizer and BioNTech that will cover 6.4 million Malaysians or 20 percent of its population of 32 million people.
In this instalment of KiniGuide, we look into this first of many Covid-19 vaccines bound for Malaysia, particularly with regard to safety.
For the record, Malaysia is also procuring a Covid-19 vaccine from AstraZeneca and is finalising deals with other manufacturers such as Sinovac, CanSino Biologics and the Gamaleya Centre.
Who or what are Pfizer and BioNTech?
Pfizer is an American pharmaceutical giant and BioNTech is a German biotechnology company. The duo collaborated to develop a Covid-19 vaccine that uses messenger RNA (mRNA or messenger ribonucleic acid).
In November last year, they announced that their vaccine candidate had 95 percent efficacy in a Phase III trial and subsequently published their findings in the New England Journal of Medicine.
Officially, the vaccine is known as 'BNT162b2'.

How does the vaccine work?
The basis of the Pfizer-BioNTech vaccine is its mRNA.
Simply put, many vaccines introduce a virus into the system to generate antibodies but this vaccine contains genetic instructions which make the body mount an immune response without the introduction of the virus.
Contrary to some claims circulating on the Internet, an mRNA vaccine does not alter a person’s DNA.
The human body already uses its own mRNA for certain cellular processes. It is temporary in nature and is destroyed after use, as such the vaccine will be no different.
How is this vaccine administered?
By injection of one dose to the upper arm, followed by a second dose 21 days later.
How safe is the vaccine?
As the University of Texas epidemiologist Katelyn Jetelina puts it: “The Pfizer vaccination gives more adverse events than the flu vaccination but less than the shingles vaccine.”
According to the report by Pfizer and BioNTech on their clinical trial, there was no meaningful difference in the rate of severe adverse events between those who received a vaccine (0.6 percent), versus those who received a “dummy” injection of saltwater (0.5 percent).
This is out of 43,252 participants enrolled in the trial, about half who were assigned to receive the vaccine while the other half received the dummy treatment.
Milder reactions typical for a working vaccine are more common, since they are designed to provoke an immune response. These include fatigue, headache, muscle pain, chills, joint pain and fever.
Such reactions are more common among younger people, especially after the second dose. In most cases, these reactions dissipated in a couple of days.
Following the vaccine rollout in the UK and the US, however, there had been reports that some vaccine recipients also suffered severe allergic reactions.

At a briefing to a panel of external experts reporting to the US Food and Drugs Administration (FDA), Pfizer representatives told the FDA on Dec 10 last year that allergic reactions were not reported in the study because people with a history of allergic reactions to vaccines were excluded from the study from the beginning.
The entire proceedings of the briefing - nearly nine hours long - was broadcasted live and is available on Youtube.
According to the US’ Vaccine Adverse Event Reporting System (VAERS), there have been seven reports of people having an allergic reaction after receiving the Pfizer-BioNTech vaccine as of Jan 1.
On Jan 6, the US Centers for Disease Control and Prevention (CDC) said allergic reactions seem to be occurring at a rate of 5.5 per 1 million vaccine doses given for both the Pfizer-BioNTech vaccine and the Moderna vaccine. These are the only two Covid-19 vaccines authorised in the US.
The CDC said these figures are still preliminary and may change
However, it also said vaccines would still be regarded as very safe even if the rate was twice as high, especially when weighed against the human cost the pandemic has already wrought.
In response to these developments, the FDA recommends that those with an allergic reaction to any ingredients of the vaccine or a previous dose of the vaccine should not get the vaccine.
In addition, it said vaccination centres should monitor vaccine recipients for immediate allergic reactions, and keep equipment on standby for treating such reactions.
It is likely that Malaysian authorities will adopt a similar approach.
For the record, VAERS is a publicly accessible database where US patients and clinicians can report adverse events that occur after vaccination.
Malaysia's National Pharmaceutical Regulatory Agency (NPRA) has a similar system in place and publishes annual reports on the complaints it receives.
The government also plans to use the MySejahtera app to collect reports on adverse reactions suspected to be linked to Covid-19 vaccines.
How effective is this vaccine?
The Pfizer-BioNTech clinical trial reported an efficacy rate of 52 percent after the first dose and 95 percent after the second dose.
The benefits begin to become apparent about 14 days after the first dose.
This is much higher than the 50 percent benchmark set by the World Health Organization, which it deems to be the minimum acceptable efficacy for a Covid-19 vaccine.
In concrete terms, this meant 170 participants in the Pfizer-BioNTech clinical trial contracted Covid-19 after at least seven days have passed after the second dose.
Upon analysis, researchers found that only eight of the infected had received the vaccine, while the other 162 received the dummy injections.
They found there was no meaningful difference in efficacy regardless of the participants' age, sex, race, ethnicity, obesity, or pre-existing medical conditions.
How long does the protection last?
This is still unknown, pending further research. So far, there is only enough data available to ascertain the vaccine's efficacy for the first two months after injection.
If it wanes too quickly, a booster shot may be needed in the months or years after the second dose.
The Pfizer-BioNTech clinical trial is designed to monitor participants for two years, including for potential safety issues that may arise in the future.
How was it developed so quickly?
This boils down to reduced red tape, increased funding, and an ample supply volunteers signing up for vaccine trials. All these factors come together to ensure researchers can spend more time working and less time waiting.
Health systems specialist Dr Khor SK explained that much of the ten-year timeline for developing a typical vaccine is spent waiting for funding to come through and waiting for various committees to meet and grant the necessary approvals, rather than conducting research.
In contrast, governments and philanthropies have channelled more money into Covid-19 vaccine research than any other branch of science in 2020.
Scientists were also able to build on previous research on vaccines and older coronaviruses, and there was a much greater degree of data sharing and competition to create the Covid-19 vaccine than other vaccines.

In addition, researchers at Pfizer, Moderna, and AstraZeneca were each able to recruit tens of thousands of volunteers for their respective clinical trials.
Khor said such large numbers usually take two to five years to recruit, but finding volunteers in the middle of the Covid-19 pandemic was much easier.
“This vaccine is a triumph of science. After NPRA approvals, we should be confident in its safety.
“Although only a year, it was very well spent. It proves that clever scientists can achieve wonders, if given enough money and political will.
“I will take the vaccine happily,” he wrote in an opinion piece published in Science Media Centre Malaysia.
Why are children excluded from receiving the Covid-19 vaccine?
The current crop of Covid-19 vaccines have yet to be tested on children under the age of 12, or in some cases, the tests are still ongoing and have yet to yield any results.
In the case of the Pfizer vaccine, for example, the youngest participants are 16 years old.
But the children are still exposed without the vaccine. How can they be protected?
The government aims to vaccinate at least 70 percent of Malaysia’s population to achieve herd immunity against Covid-19.
If a sufficient proportion of the population becomes immune to Covid-19, this would impede the spread of the disease to those who remain susceptible to infection.
The healthcare system would also be under less strain and would be better prepared to treat the cases that arise after a successful mass vaccination campaign, as well as ailments other than Covid-19.
All these would bring Malaysia a step closer towards normalcy, or at least avoid having to resort to less-palatable measures to avert a collapse of the healthcare system.

Is it compulsory?
No. Science, Technology and Innovation Minister Khairy Jamaluddin said Covid-19 vaccination will be voluntary.
Do I have to pay for the vaccine?
The vaccines will be made available for free to any Malaysian who wants it.
Khairy Jamaluddin said the government is also considering whether to provide free vaccination for migrant workers, to help achieve the herd immunity target.
Migrant worker hostels have been the epicentre of several large Covid-19 outbreaks in the country.
Has it been approved?
Not yet. Pfizer had submitted its dossier for NPRA’s evaluation on Dec 15 last year.
The NPRA would assess it for quality control, efficacy, and safety before making recommendations on the vaccine.
The Health Ministry aims to do this in less than 90 days, compared to the typical period of 90 to 120 days.
Who will get the vaccines first?
The Special Vaccine Supply Access Guarantee Committee is expected to announce a vaccine rollout plan sometime this month. The plan was slated to be finalised on Jan 7 and presented to cabinet on Jan 17.

Khairy, who co-chairs the committee, said frontliners such as Health Ministry staff, police, armed forces, Immigration Department personnel and others will be among the first.
Older folk and those with chronic diseases will also sit higher on the priority list as they are more susceptible to the worst effects of Covid-19 including a higher mortality rate.
Those interested in the vaccine will be able to register their interest through the MySejahtera app and also use the app to monitor any side effects that may arise.
For the record, of the 12.8 million doses of the Pfizer-BioNTech vaccine, one million doses are expected to arrive by the first quarter of this year.
Another 1.7 million doses are to be delivered in the second quarter, 5.8 million in the third quarter and 4.3 million in the fourth quarter.
Malaysia also has an option to order an additional 12.8 million doses from Pfizer in case other vaccine vendors fail to make deliveries.
What should you tell the doctor before you receive the jab?
According to FDA, you should inform the doctor if you have any of the following - allergies, a fever, a bleeding disorder or if you are on a blood thinner, if you are immunocompromised or are on medication that affects your immune system, are pregnant or plan to become pregnant, breastfeeding or have received another Covid-19 vaccine.
Its Malaysian counterpart has yet to issue any guidance on the matter as it is still evaluating the vaccine.
This instalment of KiniGuide was compiled by FAISAL ASYRAF.


